
How AI and Automation Are Changing Revenue Cycle Management Workflows
Revenue cycle management (RCM) in healthcare has never been more complex. Payer rules shift constantly, compliance demands grow, and operational inefficiencies eat directly into reimbursement. For practices running on thin margins, AI-driven medical billing and RCM automation have moved from nice-to-have to essential.
Artificial Intelligence (AI) and automation are transforming RCM workflows into streamlined, data-driven systems that improve accuracy, reduce administrative burden, and accelerate reimbursements.
FutureMD leverages this shift by combining automation with expert-led services, enabling healthcare providers to optimize both clinical and financial outcomes.
The Growing Complexity of Revenue Cycle Management
RCM encompasses the entire financial lifecycle of a patient encounter, from appointment scheduling and insurance verification to claims submission, payment posting, and final collections. Each stage involves multiple touchpoints, data exchanges, and compliance requirements.
Healthcare practices commonly face challenges such as:
- High claim denial rates
- Delayed reimbursements
- Coding inaccuracies
- Administrative overload
- Fragmented workflows across systems
Without optimization, these inefficiencies lead to revenue leakage, increased days in accounts receivable (A/R), and reduced operational productivity.
AI and automation directly address these pain points by streamlining workflows and enhancing decision-making across the revenue cycle, strengthening the impact of modern revenue cycle management services for healthcare providers.
AI-Driven Transformation Across the RCM Lifecycle
AI is transforming the entire RCM lifecycle by automating workflows and improving efficiency at every stage.
1. Intelligent Patient Access and Eligibility Verification
The revenue cycle begins before the patient even enters the clinic. AI-powered systems can automate insurance eligibility verification, benefits checks, and patient data capture. These tools cross-check payer databases in real time, so front-desk staff have accurate coverage information before the patient is seen.
This reduces front-desk workload, minimizes eligibility-related claim denials, and improves patient transparency through upfront cost estimates.
FutureMD strengthens this process by integrating benefits verification across phone, fax, and digital channels, helping ensure accurate coverage determination and improving clean claim performance.
2. Automated Medical Coding and Charge Capture
Medical coding directly impacts reimbursement accuracy. AI-driven systems use natural language processing (NLP) to analyze clinical documentation and assign appropriate codes.
Key benefits include:
- Improved coding accuracy and compliance
- Reduced risk of undercoding or overcoding
- Faster charge capture
FutureMD combines AI tools with certified coding specialists to ensure clinical accuracy and optimal reimbursement outcomes, an essential component of high-quality medical billing services.
3. Streamlined Claims Submission and Processing
AI-enabled platforms automate claims submission, ensuring claims are accurate and compliant before reaching payers. This improves first-pass acceptance rates and reduces delays.
Automation also accelerates reimbursement timelines, improving cash flow predictability.
FutureMD supports this with dedicated claims workflows, ensuring timely submission, continuous monitoring, and quick error resolution to maximize reimbursement.
4. Predictive Denial Management and Appeals
AI-driven analytics help identify patterns in claim denials and address issues proactively.
Key capabilities include:
- Identifying high-risk claims before submission
- Automating denial categorization
- Streamlining appeals
This approach reduces rework, improves recovery rates, and protects revenue.
FutureMD’s RCM model incorporates both predictive insights and hands-on payer follow-up. Our specialized team manages denial rework, appeals, and payer communication, ensuring that unresolved claims are actively pursued and converted into revenue rather than written off.
5. Automated Payment Posting and Reconciliation
Payment posting is often time-intensive, especially for paper remittances. Automation extracts and matches payment data with claims, ensuring accurate posting.
This improves financial visibility and enables faster reconciliation of outstanding balances.
FutureMD supports this workflow by managing detailed payment posting processes, including manual and electronic remittances. By ensuring accurate reconciliation and timely updates to financial records, practices gain better visibility into cash flow and accounts receivable performance.
6. Enhanced Patient Billing and Engagement
AI-powered billing tools improve patient engagement through automated communication, reminders, and digital payment options.
Key features include:
- Automated patient notifications
- Online payment portals
- AI-assisted support
These capabilities improve collection rates while enhancing the patient financial experience.
FutureMD extends this capability through its inbound patient call center and billing support services. Patients can directly engage with trained representatives for billing inquiries and payment processing, ensuring a smoother financial experience while improving overall collection efficiency.
The Role of AI in Strategic Financial Decision-Making
Beyond operational automation, AI provides actionable insights through advanced analytics. Healthcare practices can leverage real-time dashboards to monitor key performance indicators such as:
- Days in Accounts Receivable (A/R)
- Claim denial rates
- Collection efficiency
- Revenue trends
Predictive analytics further enables practices to forecast revenue, identify inefficiencies, and make informed strategic decisions. This data-driven approach supports long-term financial sustainability and growth.
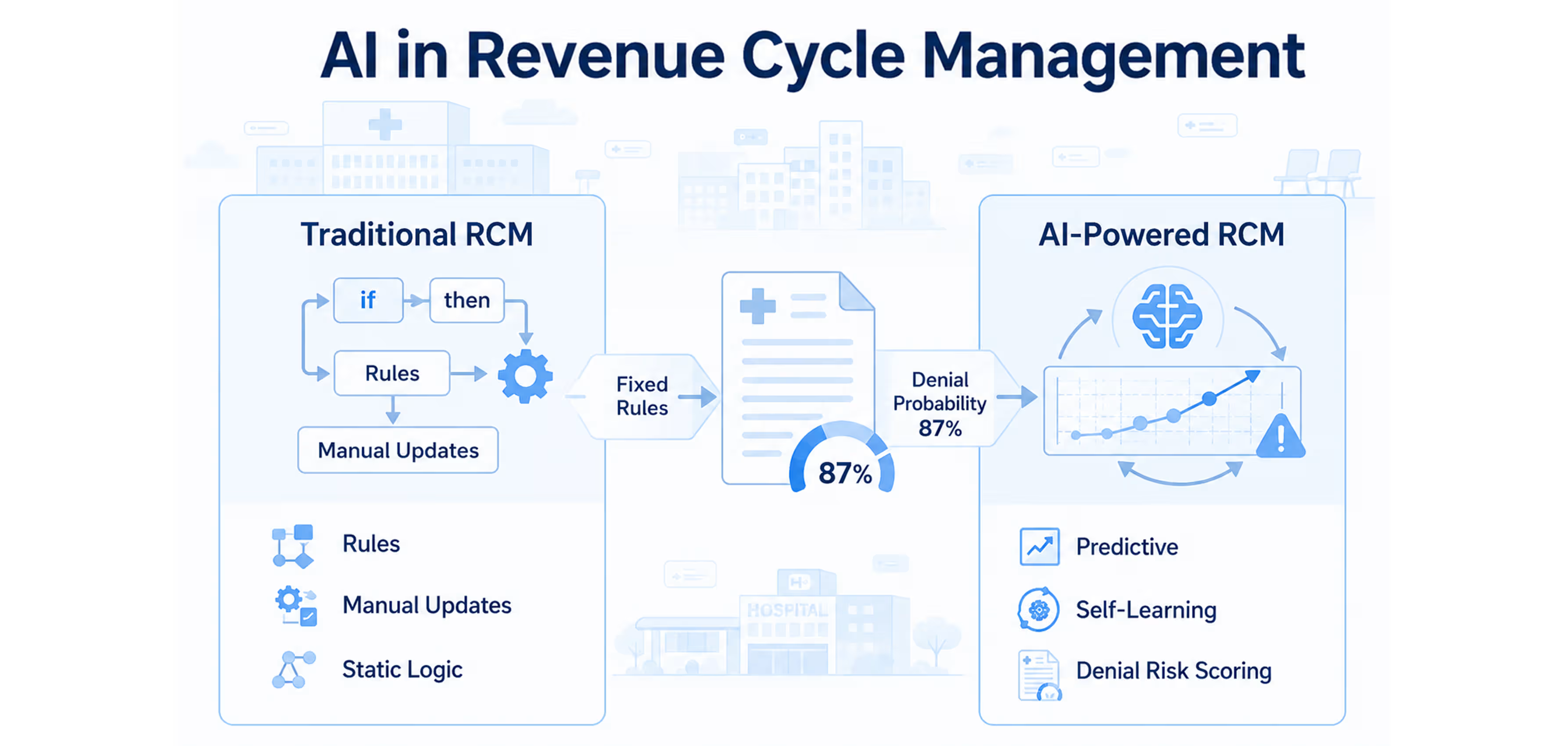
FutureMD: A Technology-Driven RCM Solution
As AI and automation reshape healthcare, revenue cycle management is evolving into a more integrated, intelligence-driven process. Solutions like FutureMD Concierge combine advanced automation with expert-led support to improve operational efficiency and financial performance.
FutureMD’s revenue cycle management services for healthcare enable providers to shift complex billing and administrative tasks to a specialized team, allowing practices to focus on patient care while maintaining consistent cash flow and revenue predictability.
Comprehensive and Flexible RCM Support
FutureMD offers a flexible, consultative approach that integrates seamlessly with existing EHR and practice management systems. Its end-to-end revenue cycle management services for healthcare providers optimize every stage of the revenue cycle from patient access to reimbursement, ensuring accuracy, compliance, and efficiency.
By combining technology with dedicated back-office expertise, FutureMD reduces administrative burden, enhances transparency, and supports scalable growth for healthcare organizations.

End-to-End Revenue Cycle Optimization
FutureMD’s approach extends beyond traditional medical billing services by addressing both front-end and back-end operations.
Front-End Optimization
- Benefits verification to ensure accurate coverage details
- Prior authorization to secure timely approvals
- Credentialing support with government and commercial payers
These processes reduce claim rejections and improve reimbursement timelines from the outset.
Back-End Revenue Management
- Accurate claims submission and follow-up
- Payment posting and reconciliation
- Denial management and appeals
- Patient billing and collections
A specialized back-office team handles these functions, reducing administrative burden and improving operational efficiency.
Advanced Support Services for Revenue Growth
FutureMD goes beyond standard RCM by offering additional services that directly impact financial performance:
- Contract and payer negotiations to optimize reimbursement rates
- Out-of-network billing management
- Worker’s compensation claim handling
- Inbound patient call center support for billing inquiries
These services ensure that healthcare practices capture every dollar across the revenue cycle.
Technology-Driven Efficiency with Human Expertise
FutureMD combines AI-powered automation with experienced billing professionals and certified coders. Intelligent automation tools, including AI-driven microbots, enhance workflow efficiency while maintaining human oversight and accountability.
This hybrid approach ensures:
- High accuracy in claims processing
- Reduced administrative workload
- Faster reimbursement cycles
- Improved compliance with regulatory standards
Aligning RCM with Value-Based Care
Modern healthcare is shifting toward value-based care models, where reimbursement is tied to patient outcomes rather than service volume. AI-driven revenue cycle management services for healthcare support this transition by aligning financial processes with quality and compliance metrics.
FutureMD’s integrated ecosystem connects Electronic Health Records (EHR), practice management, telehealth, and RCM into a unified platform. This enables healthcare practices to streamline workflows, reduce costs, and improve both clinical and financial outcomes.
Key Takeaways: Why AI-Driven RCM Matters Now
AI and automation are now essential in revenue cycle management, enabling healthcare practices to improve efficiency, accuracy, and financial stability through data-driven workflows and reliable medical billing services.
Solutions like FutureMD Concierge combine technology with expert support to streamline the entire revenue cycle from patient access to reimbursement, reducing administrative burden and improving cash flow. For healthcare providers, adopting AI-driven RCM is key to building a scalable, resilient, and future-ready practice.
Experience the impact of advanced, technology-driven revenue cycle management services for healthcare. Schedule a free consultation with FutureMD.
FAQs
1. What is AI-driven revenue cycle management?
AI-driven revenue cycle management (RCM) uses artificial intelligence and automation to optimize every stage of the billing process, from patient intake and eligibility verification to claims submission, denial management, and payment posting. These systems analyze data in real time, reduce manual tasks, and improve accuracy, helping healthcare providers streamline workflows and maximize revenue.
2. How does AI reduce claim denials in medical billing?
AI reduces claim denials by identifying errors and risks before claims are submitted. It can flag missing information, coding inconsistencies, and payer-specific requirements, ensuring cleaner claims. Also, predictive analytics helps detect patterns in past denials, allowing practices to proactively correct issues and improve first-pass acceptance rates.
3. Is AI medical billing HIPAA compliant?
Yes, AI medical billing solutions can be fully HIPAA compliant when implemented correctly. Reputable platforms follow strict data security protocols, including encryption, access controls, and secure data handling processes. Compliance ultimately depends on using certified systems and maintaining proper safeguards around patient information.
4. How much can automation reduce RCM costs?
Automation can significantly reduce RCM costs, often by 20% to 40%, by minimizing manual work, reducing errors, and accelerating reimbursements. It lowers administrative overhead, shortens accounts receivable cycles, and improves staff productivity, allowing healthcare organizations to operate more efficiently while maintaining accuracy.